No Fee Unless You Win
No Fee Unless You Win
Traumatic brain injury (TBI) is a major cause of death and disability in the United States. Every year there are around 3 million TBI-related emergency department (ED) visits, hospitalizations, and deaths. Nearly 150 Americans die from TBI-related injuries each day. Those who survive a TBI can face effects that last a few days or the rest of their lives.
This guide is provided by Gage Mathers to help those who suffered a traumatic brain injury (also known as a TBI). The material presented is largely adapted from the CogSMART program of the VA San Diego Healthcare System with the permission of Elizabeth W. Twamley, Ph.D., Professor of Psychiatry at UC San Diego. CogSMART focuses on cognitive training to help people improve skills that are impaired by TBIs. Since many TBIs go undiagnosed or undertreated, we hope this guide will empower you to have your health care providers test for TBI and, if you have one, to quickly get you the help you need.
Download the TBI & Post-Concussion Syndrome Screening Questionnaire
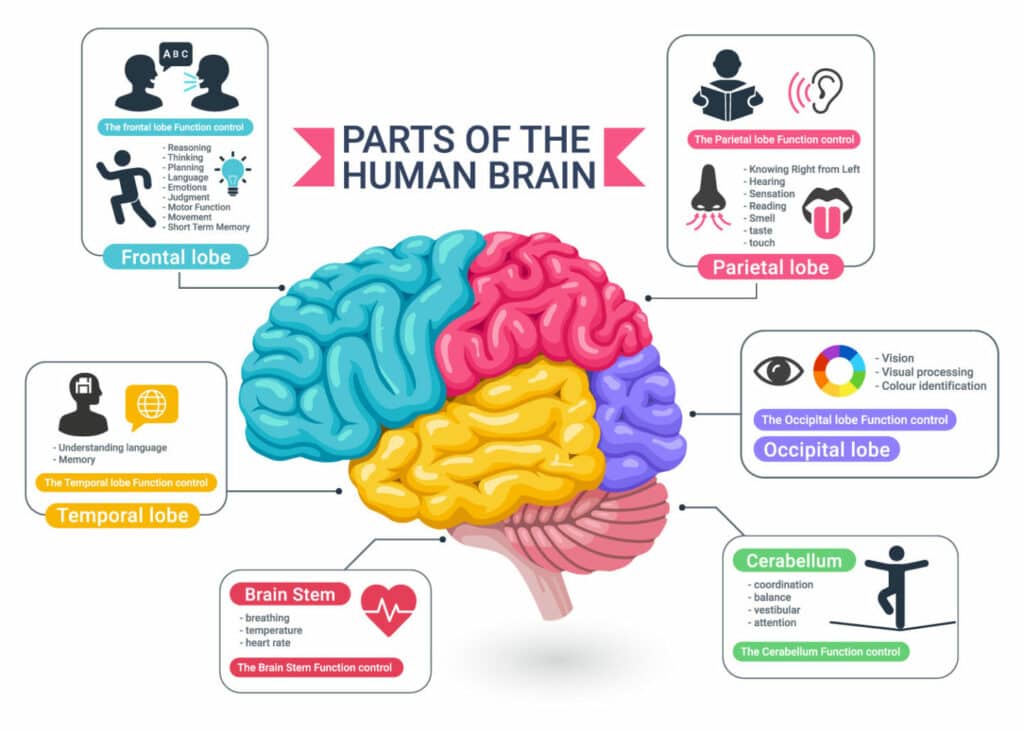
What is traumatic brain injury (TBI)?
A TBI is basically a disruption in the normal function of the brain that can be caused by a bump, blow, or jolt to the head, or penetrating head injury like a gun shot. TBIs of all degrees can cause impaired physical, cognitive, emotional, and behavioral functioning.
A “mild” TBI may affect your brain cells temporarily, like a concussion. A “moderate” or “severe” TBI can result in bruising, torn tissues, bleeding, and other physical damage to the brain causing long-term complications, like coma, or death.
What causes TBI?
The most common causes of TBI in the United States are:
Falls are the leading cause and account for almost half of all TBI-related emergency department visits. Car accidents are second.
When an individual suffers a TBI, the brain can be injured in a number of different ways. For example, the brain may be shaken within the skull causing bruises (also called contusions) to form at the sites of impact. Like bruises elsewhere on the body, these will heal with time. Swelling may occur if there are many bruises on the brain, which can take a while longer to return to normal.
Brain injury can occur even when there is no direct blow to the head, such as when a person suffers whiplash. When the head is rapidly accelerated and decelerated, as in a car accident, twisting or rotational forces may stretch and even sever long-range connecting fibers in the brain. Damage to these fibers disrupts communication between nerve cells and, thereby, reduces the efficiency of widespread brain networks.
Damage to blood vessels surrounding the brain is another common source of injury, causing bleeding between the brain and skull. This bleeding often stops on its own and the blood vessels heal like any other cut.
Exposure to rapid pressure changes, such as the overpressurization and underpressurization waves that accompany explosions, can also cause damage to the brain. These pressure shifts induce air bubbles to form in the bloodstream, which can then travel to the brain and interrupt its blood supply. These types of TBIs are more frequent in the military, seen in as many as 20% of non-fatal military injuries. As a result, TBI has become known as the “signature wound” of Operation Enduring Freedom” (the war in Afghanistan) and “Operation Iraqi Freedom” (the war in Iraq).
The severity of TBI can range from “mild” (characterized by relatively brief changes in mental status or consciousness following the injury) to “severe” (characterized by an extended period of unconsciousness or amnesia after the injury). Thus, the length of time that a person is unconscious is one way to measure the severity of the injury. If you were not knocked out at all or if you were unconscious for less than 30 minutes, your injury was most likely minor or mild. If you were knocked out for more than 30 minutes but less than 6 hours, your injuries were probably moderate.
Approximately 80% of TBI cases are classified as mild, with emergency department visits for mild TBI (mTBI) topping two million each year. Although this is a very high number of cases, there may even be more mTBIs because a number of cases go unreported or undetected. mTBIs are especially difficult to diagnose because these individuals typically do not show obvious physical signs of injury (e.g., skull fracture), and rarely display evidence of brain damage on neuroimaging exams.
The term “mild” may be misleading in reference to brain injury. Although someone may only be dazed or confused or have a brief loss of consciousness in mTBI, evidence of impaired brain function is often clear. Cognitive changes, headaches, dizziness, and a number of other symptoms may be observed following mTBI. The actual harmful effects on the daily functioning of persons with mTBI may be large depending on what type of activities that person must do on a daily basis. Not all symptoms will quickly resolve or go away without treatment.
Diagnosis of TBI is difficult because affected individuals may not show physical signs of injury. Even sophisticated neuroimaging techniques may fail to detect signs of brain injury. Tests such as EEG, CAT scans, and MRIs are often “normal.” Typically, only relatively large abnormalities are detected by current imaging techniques. Neuropsychological testing may be performed in cases of suspected TBI and can be an effective method of identifying associated cognitive deficits.
A comprehensive neuropsychological battery takes several hours to administer and includes a broad range of tests. On formal testing, persons with TBI may show problems with information processing speed, memory, and distractibility. Around one month post-injury, the effects are usually mild in young persons with no previous problems with health or thinking. But for some people, symptoms can last for days, weeks, or longer. In general, recovery may be slower among older adults, young children, and teens. Those who have had a TBI in the past are also at risk of having another one. Some people may also find that it takes longer to recover if they have another TBI.
TBI can have wide-ranging physical and psychological effects.
mTBI symptoms include:
| Thinking/ Memory |
Physical | Emotional/ Mood |
Sleep |
| Feeling dazed, confused, or disoriented (early on) | Nausea or vomiting (early on) | Irritability | Sleeping more than usual |
| Difficulty thinking clearly | Headache | Sadness | Sleep less than usual |
| Difficulty concentrating | Sensitivity to noise or light | More emotional | Trouble falling asleep |
| Difficulty remembering new information | Feeling tired, having no energy | Nervousness or anxiety | |
| Difficulty speaking | Fuzzy or blurry vision | Feeling depressed | |
| Feeling slowed down | Dizziness | ||
| Balance problems | |||
| Ringing in the ears | |||
| Bad taste in mouth or changes in ability to smell |
Infants and young children with brain injuries might not be able to communicate headaches, sensory problems, or confusion. Therefore, monitor infants and children for:
Whether in adults or children, these symptoms are part of the normal recovery process and are not necessarily signs of brain damage or medical complications. They are part of a constellation of symptoms called post-concussion Syndrome (PCS). These symptoms are expected as you get better. The majority of patients with PCS recover completely in 3 to 6 months. For a minority of patients, approximately 20%, symptoms may persist for a longer period of time. Most patients don’t develop PCS symptoms until days or even weeks after the accident, but the syndrome can begin sooner. Either way, the symptoms often disappear without any special treatment. A list of some of the symptoms you can expect is shown below, along with the percentage of head-injured patients who experience each symptom at some point during their recovery.
Symptoms of Post-concussion Syndrome
<td”>Percentage <td”>80%<td”>71%<td”>66%<td”>64%<td”>63%<td”>59%<td”>59%<td”>58%<td”>57%<td”>52%<td”>45%<td”>40%
| Symptom |
| Sleep difficulties |
| Poor concentration |
| Irritability |
| Fatigue |
| Depression |
| Memory problems |
| Headaches |
| Anxiety |
| Trouble thinking |
| Dizziness |
| Blurry or double vision |
| Sensitivity to bright light |
When unrecognized and untreated, these symptoms often disrupt the individual’s work setting and family relationships. People frequently report feeling as though they are “going crazy.” Healthcare providers may consider them overanxious and, therefore, fail to diagnose TBI.
Moderate to severe TBI symptoms can include any of the symptoms of mTBI, as well as these symptoms that may appear within the first hours to days after a head injury:
| Thinking/ Memory |
Physical | Emotional/ Mood |
Sleep |
| Profound confusion | Persistent headache or headache that worsens | Agitation | Sleeping more than usual |
| Slurred speech | Repeated vomiting or nausea | Combativeness | Inability to wake up |
| Coma | Convulsions or seizures | Unusual behavior | |
| Dilation of one or both pupils | Worsening depression | ||
| Weakness or numbness in fingers and toes |
In rare cases, a dangerous blood clot that squeezes the brain against the skull can develop. Take the injury victim to the emergency department immediately if they have signs or symptoms of a moderate to severe TBI, especially:
What can I do about these symptoms?
The main treatment is rest and over-the-counter pain relievers.
PCS is a normal part of recovery. Most patients return to normal by 3 months without any special treatment, although rest is often necessary. The symptoms are not a sign of relapse or brain damage. The syndrome is expected even after minor head injury. Few patients will experience all of the symptoms, but even one or two of the symptoms can be unpleasant.
Some patients find that at first, PCS makes it hard to work, get along at home, or relax.
The best way to deal with this is to resume activities and responsibilities gradually, a little at a time. The time you spend at work, getting together socially, with your family, or exercising should be determined by what you are comfortable with. You should pace yourself and be sure to get all the rest you need. If your symptoms get worse, or if you notice new post-concussion symptoms, this could be a sign that you are pushing yourself too hard or your condition is worsening. Ignoring your symptoms and trying to “tough it out” often make the symptoms worse and can prolong your recovery.
Symptoms are your body’s way of giving you information. For instance, a broken bone or a torn muscle hurts so that you won’t use it and it has time to heal. Post-concussion syndrome is your brain’s way of telling you that you need to rest your brain. Most doctors who treat head injuries agree that recovery is faster when the patient gets enough rest and resumes responsibilities gradually. Scientific studies suggest taking a full week of rest and then gradually increasing activity can shorten symptoms by up to two months.
Thinking and worrying about your symptoms can make them seem worse. This is partly because paying attention to a feeling seems to magnify or increase it. Generally, focusing on a symptom tells your brain that it is important enough to block out perception of other things, or even amplify the symptom in your mind. Therefore, it is important to remember that the symptoms are a normal part of recovery and will likely go away on their own.
Don’t forget that we all have some of these symptoms once in a while. After a head injury it can be easy to forget that we were sometimes irritable, tired, had headaches, couldn’t concentrate, or forgot things even before the accident. Thus, some of the symptoms you notice may actually have nothing to do with your head injury. The symptoms of PCS are pretty much the same as the symptoms of ordinary day-to-day stress. Here is a list of symptoms along with the percentage of people who experience each symptom even though they did not have a head injury:
Symptoms of Everyday Stress
| Symptom | Percentage |
| Poor concentration | 18% |
| Irritability | 30% |
| Fatigue | 25% |
| Depression | 14% |
| Memory problems | 20% |
| Headaches | 60% |
| Anxiety | 30% |
| Trouble thinking | 10% |
| Dizziness | 5% |
| Blurry or double vision | 8% |
| Sensitivity to bright light | 14% |
The reason that the symptoms of PCS are so much like the normal signs of daily stress is that one main cause of these symptoms is exactly the same: everyday stress. Of course, your TBI has a lot to do with it, but having a head injury adds more stress to your life, not just bumps and bruises to your head. The accident itself, being in the hospital, going back to work or school, and trying to schedule follow-up appointments are all things that add stress to most patients’ lives. Bills can pile up, time is lost, and there may be injuries to other parts of your body. And just like a pulled muscle or bruised leg, your brain takes some time to recover. You may have some trouble with work or school at first, and this increases your stress and frustration. Just remember, it takes some time to get better.
Another main cause of stress after a head injury is worry about the symptoms you have. Scientific studies by neurosurgeons and neuropsychologists in New Zealand show that patients who read an information guide, like this one, recover faster and feel better during recovery than patients who do not know what to expect. That’s why we created this guide.
Poor Concentration
The main cause of poor concentration is tiredness. When it becomes difficult to concentrate on what you’re doing, take a break and relax. Between 15 and 30 minutes a day should be enough. If you still continue to have problems, your workday, class schedule, or daily routine should be temporarily shortened. Trying to “stick to it” won’t help, and usually makes things worse.
Reducing distractions can help. Turn down the radio or try to work where it’s quiet. At first, avoiding noisy environments may be helpful, then return to them gradually. Don’t try to do too many things at once. Writing while you talk on the phone or taking notes as you listen to someone are examples of doing two things at the same time. It may be difficult for you to concentrate on more than one thing at first. You will be better able to concentrate when you’ve had enough rest. So, if you really need to concentrate on something important, do so when you’re feeling fresh.
Fatigue
It is normal to be more tired after a head injury. Most people experience some degree of fatigue during their recovery. The only sensible treatment for being tired is rest. Avoid wearing yourself out. Gradually increase your activity level. You may find that you need to sleep more than usual, in which case it is a good idea to get the extra sleep that you need. Most patients have more energy in the morning than later in the day. An afternoon nap can help if you find that it is harder to do things at the end of the day. Physical and mental fatigue usually diminishes over time; it should be greatly improved within 6 months after a brain injury.
It may seem counterintuitive, but a well-designed exercise program can help your physical and mental endurance. Adding activity gradually is the key. For instance, an hour of morning activity may be all that you can handle. From there, you slowly and incrementally add activity followed by rest breaks. Closely monitor your fatigue levels until you reach an acceptable level that you can tolerate. Be careful to avoid extreme fatigue.
| Simple suggestions to reduce fatigue: |
|
Sleep Difficulties
You might expect that the fatigue you experience during recovery will cause you to sleep more soundly. However, sleep disturbance is actually quite common following a brain injury. Studies have shown that individuals who suffer a brain injury often have difficulty getting to sleep and maintaining uninterrupted sleep at night, and thus experience excessive daytime sleepiness. When they do sleep, their sleep is lighter and less restful, and they frequently awaken.
Getting adequate sleep is very important in the healing process. If you don’t sleep well at night, you’ll be more tired during the day. When you’re tired during the day, you’ll find it difficult to concentrate and may become irritable and angry more easily. Thus, lack of sleep can exacerbate your other symptoms.
| Simple suggestions to improve your sleep habits and routines: |
|
Irritability and emotional changes
Some people show emotions more easily after a brain injury. They may yell at people or say things they wouldn’t normally say. They may get annoyed easily by things that normally would not upset them, or are easily frustrated and even become tearful. Some may even get violent. These unusual behaviors occur because the brain is not regulating emotions to the same extent as before the injury. If any of these episodes happen, it is usually a sign that it is time to take a rest from what you are doing and get away from it.
There are a variety of different techniques to deal with irritability. Some people find that leaving the frustrating situation temporarily is helpful. Others employ relaxation techniques or attempt to use up emotional energy through exercise. One frequent cause of irritability and emotionality is fatigue. People lose their tempers more easily when they are tired or overworked. Adjust your schedule and get more rest if you notice yourself becoming irritable or emotional.
Everyone gets angry from time to time, often with good reason. Being irritable only becomes a problem when it interferes with your ability to get along with people from day to day. If you find yourself getting into arguments that cause trouble at home or work, try to change the way you think about things. Try imagining an irritating situation and why it would make you angry. There is usually a reason that irritating things happen. When something makes you angry, ask yourself what caused it. Family, friends, or co-workers can do things that bother us at times. Try to think of why they did whatever it was that irritated you. What would they say the reason was? Thinking about what caused a problem is the first step toward solving it.
Problems can usually be solved better if you stay calm and explain your point of view. The steps you need to take to solve a problem will be the same when you are calm as they would be if you were irritated. Try to remind yourself of this when you find yourself becoming irritable.
You can usually come up with several ways to solve a problem. Try to think of at least five different ways, and then decide on which is best. Just realizing that there are several things you can do to solve a problem will make it a lot less irritating.
Depression
For reasons we do not fully understand, depression seems to occur more often after a brain injury. More than one-third of people with recent TBI become depressed, especially during the first year after injury. One reason for this increase in depression may be that brain injury causes an imbalance in certain chemicals in the brain and disrupts brain networks critical for mood regulation.
Another cause of depression in TBI may be psychological and social changes such as losing friends, losing abilities, and not being able to return to work or other meaningful activities after injury. Simply put, people become depressed when unpleasant things happen to them, and a head injury is unpleasant. We feel good when good things happen to us. Thus, an effective way to treat depression is to make sure that good things happen. One way to do this is to plan to do something enjoyable for yourself each day. Make your plan specific, and then be sure to stick to it. Decide on an activity you like and exactly when you are going to do it. That way you can look forward to it. Anticipating and doing enjoyable things each day will improve your mood.
Chances are that if you are depressed, you are telling yourself things that are depressing. Thinking that the situation is terrible, that there is no end to it in sight, that you aren’t able to do anything about it, and that it is your fault are all depressing things to tell yourself. Thinking this way can become a habit if you do it enough. Usually, when people tell themselves unpleasant things all the time it is out of habit, not because those things are really true. If you find yourself thinking depressing thoughts, stop. Simply stopping a depressing thought can make you feel better. See if what you are telling yourself is really true.
Memory problems
Memory difficulties have several causes. The part of our brain that stores memories is called the temporal lobe. This is the part of the brain that is most likely to be bruised in a head injury. Some memory difficulties can be caused by the bruises, which is why you may not remember the accident very well. Like a black and blue mark on your arm or leg, these bruises will recover with time. Your memory will most likely improve as this happens.
Most of the memory problems that patients notice after a head injury are not caused by bruising. They usually come from poor concentration and being tired. For you to remember something, you have to pay attention to it first. If you don’t concentrate long enough, the information is never stored in your memory. Concentration problems are a normal part of recovering from a head injury and some memory trouble is a normal side effect of this. You will probably be able to concentrate and remember better when you get enough rest. Memory problems can be a sign that you are pushing yourself too hard. Writing important things down, using a pocket tape recorder, and asking for reminders are other excellent ways of coping with temporary memory difficulties. They will help recovery and not slow it down.
Of course, nobody’s memory is perfect anyway. After a head injury, it can be easy to forget that we sometimes had trouble remembering things even before the accident. Some of the symptoms you notice may actually have nothing to do with your head injury. A list of common memory “problems” is shown below along with the percentage of people who experience each “symptom” even though they didn’t have a head injury.
Things We Normally Forget
| “Symptom” | Percentage |
| Forgets telephone numbers | 58% |
| Forgets people’s names | 48% |
| Forgets where car was parked | 32% |
| Loses car keys | 31% |
| Forgets groceries | 28% |
| Forgets reason for entering room | 27% |
| Forgets directions | 24% |
| Forgets appointment dates | 20% |
| Forgets store locations in mall | 20% |
| Loses items around the house | 17% |
| Loses wallet or pocketbook | 17% |
| Forgets content of daily conversations | 17% |
Worrying about remembering things that you would normally forget can make your memory seem worse to you. If you can remember your memory problems, you probably don’t have much of a memory problem!
People with serious memory difficulties are usually not upset by their symptoms. They don’t remember that they have any memory trouble.
Headaches
Headaches are part of the normal recovery process, but that doesn’t make them any less bothersome. Not only are they painful to experience, but frequent headaches can take a toll on you mentally and emotionally, and are a common cause of irritability and concentration problems following a head injury. This guide cannot replace the medical advice that you should get if you are bothered by headaches. Headaches can have many causes, and your doctor will want to diagnose the problem and prescribe medication that can help if you need it.
One of the most common causes of headaches after a head injury is stress or tension. This is usually the case when the headaches start for the first time several weeks after the injury. These headaches mean that you are trying to do too much. They will probably disappear if you take a break and relax. Your workday, class schedule, or daily routine should be temporarily shortened if you continue to have headaches. Stress or worry cause tension headaches by increasing muscle tension in your neck or forehead. These muscles become tense and can stay tight without you realizing it, out of habit. They can become even tighter once a headache starts because muscles automatically tense in reaction to pain. This muscle tension makes the headaches worse.
If you have tension headaches, relaxing your muscles can help. One way to do this is with a method called progressive muscle relaxation. Start by clenching your hand into a fist, as hard as you can. Notice how the muscle tension feels. Now relax your hand completely and notice the difference. Now clench both your hands as hard as you can and hold them that way for a moment or two before letting them relax completely. Notice the difference. Now continue to tense and relax more muscle groups by adding a different set each time: hands, arms, face, chest, stomach, buttocks, legs, feet. This method works best if you are lying on your back. Finally, tense all the muscles in your body at once as hard as you can, and then let them relax. At this point, all your muscles will be very, very relaxed. Progressive muscle relaxation can help prevent tension headaches by relaxing your muscles. This works best if you practice it each day at about the same time for 5 minutes or so. But, be sure that you DO NOT use this technique while you are having a headache or with a body part that is injured.
Anxiety
Worrying about symptoms and problems at work is the main cause of anxiety for many patients. Anxiety should not be a problem for you if you understand that your symptoms are a normal part of recovery, get enough rest, and gradually increase your responsibilities at work. If you are anxious, chances are that you are telling yourself things that are making you that way. Usually, when people worry all the time it is out of habit, not because the things that they are telling themselves are really true. The steps you need to take to solve a problem will be the same when you are calm as they would be if you were anxious. If you find yourself thinking anxious thoughts, stop. Simply stopping an anxious thought can make you feel better. See if what you are telling yourself is really true.
Confusion and trouble thinking
Many people feel uncertain, perplexed, or confused after a head injury. They find that their mind and feelings don’t react in the ways they used to. They may fear that they are “going crazy.” This is a normal reaction to a head injury. If you have these feelings, it is good to talk about them with someone you trust.
Trouble thinking is often a side effect of other symptoms. Concentration problems, being tired, headaches, and anxiety can all make it hard to think clearly. Like these other symptoms, trouble thinking is probably a sign that you are doing too much too soon.
Dizziness, visual difficulties, and light sensitivity
Dizziness and visual difficulties should be checked by your doctor. These symptoms usually go away by themselves in 3-6 months or less in most patients. If you find these symptoms troublesome, your doctor may want to prescribe medication for motion sickness, or eyeglasses. Some motion sickness medications are very effective for dizziness, but can make you drowsy or reduce your attention span as side effects.
You may notice some increased sensitivity to bright light or loud noise, particularly if you have headaches. Some increased sensitivity is normal after a head injury. Scientific studies show that a person’s actual sensitivity to light and noise has nothing to do with how much light and noise bother them. Paying attention to these symptoms makes them seem worse because paying attention to a feeling seems to magnify or increase it. The less you think and worry about your symptoms, the faster they will usually go away.
Are there treatments for TBI?
Research on treatment for TBI has not come up with a single treatment that is effective for all patients. Many people recover without any formal treatment. Usually, they get better rapidly in the first few days, and problems that linger may clear up in a few weeks or months. Some problems become more apparent as you return to your usual activities. For example, you may not realize that you get tired easily until you return to your usual activities. Even so, people usually get better after a head injury, not worse.
Until recently, little more than acute medical treatment was provided for survivors of mTBI. People were often discharged from emergency rooms without adequate follow-up. Today, however, rehabilitation programs are available to address cognitive retraining, psychosocial adjustment, communication and leisure skills, and vocational issues. With appropriate support and therapy, individuals with difficulties related to TBI can learn to overcome and compensate for their deficits, resulting in successful reintegration into their home and work environments. Also, there are several medications that can be used to treat symptoms like anxiety, depression, seizures, muscle spasms, and decreased attention.
Returning to school or work
Returning to school or work is often one of the most difficult phases of recovery from brain injury. This is because a number of TBI symptoms can interfere with your ability to manage the demands of work and school environments. For example, concentration difficulties and memory problems may affect your capacity to learn new things in school. Or fatigue may limit your ability to effectively handle work responsibilities throughout the day. One important thing to keep in mind when attempting to return to work or school is that the process will be gradual. It would be unreasonable to expect yourself to immediately perform at the level you were functioning prior to your TBI. Instead, you should gradually resume responsibilities as you are able. Slowly increase your workload and hours when you feel fully equipped to handle such increases.
When returning to school, be sure to find out what special help and accommodations are available to you. You may be eligible for extra test-taking time, help with note-taking, etc. A visit to your school’s “student services” or “disability services” office will help you determine the resources available and how to obtain them.
| Some general advice to aid recovery: |
|
You can find additional resources and information guides at CogSMART Manuals and Resources.
Summary
Head injuries of all types can be serious and require medical attention. From an actual impact or simple jolt, all head trauma can cause a brain injury that leads to painful and disabling symptoms. The most common symptoms after a head injury are known as post-concussion syndrome. These symptoms are part of the normal recovery process and are usually not signs of brain damage or medical complications. They are not a cause for concern or worry. Post-concussion syndrome is more common after a mild head injury. Few patients will experience all of the symptoms. The symptoms may not develop until days or even weeks after the accident. Most patients will be back to normal within 3 months without any special treatment. The key to a shorter recovery is rest, avoiding stress, not focusing on symptoms, and gradually increasing activity levels. If symptoms worsen, new symptoms develop, or symptoms correlate with a moderate to severe TBI, then you may benefit from medical intervention.
The material presented is based on published scientific research and clinical studies and was adapted from a variety of sources including:

Those who are in a car accident where the other driver flees may wonder about the hit-and-run settlement process. In many cases, full coverage policies include uninsured motorist coverage that can he...
Posted by Joseph D'Aguanno
Traffic cameras can provide critical information about a hit-and-run accident. Footage can be used by the police and your car accident attorney in Phoenix to gain an unbiased account of the befor...
read morePosted by Joseph D'Aguanno
In Arizona, the statute of limitations for filing a claim for a hit-and-run accident is the same as for other motor vehicle accidents. A victim must file a claim against the at-fault parties with...
read moreIf you or a loved one has been seriously injured, please fill out the form below for your free consultation or call us at (602) 258-0646
2525 E Arizona Biltmore Cir #A114, Phoenix, AZ 85016
get directions